Root Canal Treatment
Root Canal Treatment
What is Root Canal Treatment?
A root canal is a treatment option that is designed to repair and “save” a damaged or infected tooth, as an alternative to removing it. Advancements in techniques and equipment for root canals have made it a quicker, easier, and often nearly pain-free procedure.
What is a Root Canal?
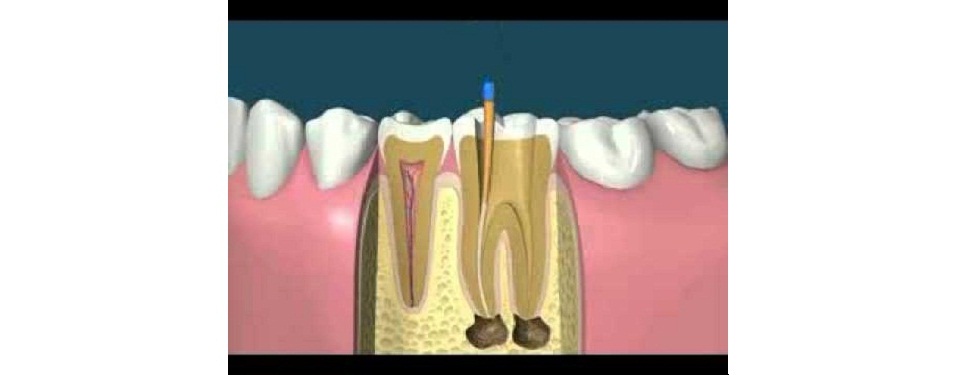
Root canal treatment is a treatment option available to “save” a tooth that has sustained damage, inflammation, or infection in the pulp, deep inside the tooth. Put simply, the damaged internal sections are removed from your tooth and replaced with material to seal the tooth. In most cases a crown is placed over the tooth to protect it from further decay and damage. Learn more about the general anatomy of a tooth.
What are the steps involved in a root canal?
Root canal procedures are often completed in two steps.
First, the dentist will numb the area to be treated, and will remove the inflamed or infected pulp. Your dentist will then clean and shape the inside of the tooth, and fill the space and seal the tooth. Your dentist may prescribe antibiotics to help heal the infection, and will often create a temporary crown or cap for the tooth. Your dentist will provide you with post procedure instructions, which include avoiding very hot or cold food or beverages, as well as chewy or hard foods or snacks for a period of time.
In some cases, your root canal may require additional structure due to the creation of the access cavity for the root canal. “Core placement” refers to a procedure where a dentist replaces missing tooth structure in preparation for making a new dental crown. Replacing these missing portions creates the optimal foundation for the new restoration. Your dentist may recommend the placement of a dental “post” to help anchor the the core material to the tooth. Learn more about post and core buildup.
Second, after the infection has cleared and the area is healing, your dentist will clean and seal the tooth again and place a permanent crown over the tooth to protect it from further damage and decay. Once the healing is complete, you should be able to return to normal use of your teeth. However, it is important to remember that dental restorations need to be proper care and maintenance to make sure they remain strong and intact.
Root Canals for Children (Pulpotomy)
A pulpotomy is the surgical removal of an inflamed pulp chamber in a child’s tooth that has been compromised due to untreated cavities and decay. Bacteria must be removed from the pulp chamber inside the child’s tooth in order to prevent or alleviate an abscess or infection. A pulpotomy is commonly referred to as a “baby tooth root canal.” A healthy tooth has a space inside it called the “pulp space” which is filled with soft tissues – nerves, blood vessels and pink connective tissue. If a tooth gets a large cavity, the bacteria in the decay can damage the pulp, which is often what causes toothache. Baby teeth are not as hard and strong as adult teeth, and the nerve inside a baby tooth is closer to the outside, which is why children are often both more sensitive and susceptible to decay and tooth pain. Learn more about pediatric pulpotomies.
Cost and Insurance Coverage for Root Canal Therapy
The cost of Root Canal therapy can vary based on the type of tooth, as well as other variables such as number of roots and any need for additional services such as Post & Core. Your dentist will review what diagnostics and treatment will be needed, and our staff will review any associated fees prior to beginning root canal therapy. If you have dental insurance, your coverage may include limited exams and diagnostics, as well as major procedures such as root canals. Our staff is happy to review your coverage with you to ensure you are maximizing your insurance benefits while minimizing any out of pocket expenses.
Signs and Symptoms
How do I know if I might need a Root Canal
Living with dental pain can be difficult. In some cases, an infection in the tooth is not always immediately painful, but the sooner you seek treatment, the better the potential outcome. It is always best to contact your dentist if you experience any of the following:
- Localized pain (can be mild to severe)
- Tooth discoloration
- Swelling or irritation around a tooth
Determination of need for Root canal treatment can only be made by a dentist or endodontic specialist. Pain, swelling, tenderness in the lymph nodes, or fever may be a sign of a true dental emergency or other serious condition and should never be ignored. If you or a loved one is experiencing any of these symptoms, we recommend you see a dental professional or visit an urgent care center right away.
Where can I get a Root Canal
Root canal treatment is a modern and very common procedure and can often be performed by a doctor, in any of our [locations]. Occasionally, however, a referral to an endodontist, or root canal specialist, for expertise in special cases.
Preparation and Post-procedure care for Root Canal Therapy (Treatment)
In many cases, your dentist can begin root canal therapy treatment right away. In some circumstances, your dentist may prescribe antibiotics and allow the infection to clear before starting treatment. There is no specific preparation needed for root canal therapy, unless you are receiving Nitrous Oxide (laughing gas) service, in which case it is recommended that you do not eat for 2 hours prior to your appointment.
Alternative Treatment options for Root Canal Therapy
If root canal therapy is not an option, alternative treatments include extraction of the tooth, with an optional replacement by a bridge or dental implant.
Frequently Asked Questions about Root Canal Therapy
I recently had a root canal and my dentist says I need to come back for a crown. I feel so much better now. Do I really need a permanent crown?
Yes. Many times patients will feel a great amount of relief from swelling or pain following the first part of the root canal treatment has been completed. However, the second step of the root canal is critical to allow your dentist to make sure the infection has cleared, and to ensure the tooth is clean and sealed to prevent any openings which may allow food particles, debris or bacteria to enter the tooth and cause further damage. The placement and [cementing] of the permanent crown is the final step to help protect the tooth and prevent future damage or even tooth loss. Completing the root canal process fully is the best way to prevent future, more costly dental emergencies and keep your smile as healthy and strong as possible.
